Diagnostics
Ted Ling Hu, Fellow
May 2023

Introduction
The history of medical diagnosis can be traced back to ancient civilizations such as Egypt, Greece, and China, where physicians relied on a combination of observation, patient history, and physical examination to diagnose diseases.[1]
The development of instruments such as the stethoscope and microscope greatly aided physicians in making more accurate diagnoses.[2, 3] Today, with advancements in technology and medical knowledge, diagnostic tools such as imaging scans, genetic testing, and biomarker analysis have revolutionized the field of medical diagnosis.

Medical diagnostics are critical in identifying the root cause of a patient's symptoms and guiding appropriate treatment. Without accurate and timely diagnosis, patients may receive inappropriate or ineffective treatments, leading to prolonged illness, complications, or even death. Furthermore, early diagnosis of diseases can lead to better outcomes, as treatment can be initiated before the disease progresses to a more advanced stage.
At Prime Movers Lab, we are deeply committed to promoting human flourishing, which has driven us to undertake an extensive exploration of the latest developments in the field of medical diagnostics. During the past 5 months, we engaged with visionary founders who are developing innovative solutions to overcome existing diagnostic challenges. Through this in-depth exploration, we identified promising trends in the diagnostics industry that could represent exciting niches for investment. This report will provide insights into these trends and highlight why we believe the diagnostics sector presents a unique opportunity for investors seeking to drive positive impact and growth.
Current Challenges with Diagnostics
Early Detection
Early detection and diagnostics are critical in the field of medicine and healthcare as they can significantly improve patient outcomes and quality of life. Early detection refers to the ability to identify a disease or condition in its earliest stages, even before any symptoms are present.[4] Early diagnosis, on the other hand, refers to the process of identifying a disease or condition based on the presence of symptoms and clinical features. Early detection and diagnosis can help healthcare professionals initiate treatment early, which can improve the chances of successful treatment and reduce the risk of complications. It can also improve patient outcomes and reduce healthcare costs. In addition to the clinical benefits of early detection and diagnostics, it also has significant implications for public health. Early detection and diagnosis can help with disease surveillance and control efforts, particularly in the case of infectious diseases, by identifying cases early on and implementing appropriate public health measures.
Accuracy and Specificity
Accuracy and specificity are important considerations in diagnostics, as they determine the reliability and usefulness of diagnostic tests.[5] The accuracy and specificity of a diagnostic test depend on a variety of factors, including the quality of the test, the prevalence of the disease in the population being tested, and the presence of other factors that may interfere with the test results. Ensuring the diagnostic is highly selective is critical but, unfortunately, it can be quite difficult to develop and commercialize a technology with both high selectivity and high specificity. It is important for healthcare professionals to carefully evaluate the accuracy and specificity of diagnostic tests before using them in clinical practice.
Access to Testing
Access to testing and diagnostics is an important challenge in healthcare, particularly in low-resource settings or areas with limited healthcare infrastructure.[6] Lack of access to diagnostic testing can lead to delayed diagnosis, inadequate treatment, and poor patient outcomes. There are several barriers to accessing testing and diagnostics, including cost, availability, and geographic location. Some diagnostic tests can be expensive, making them inaccessible to patients or healthcare systems with limited resources. Additionally, some diagnostic tests may only be available in certain geographic locations or may require specialized equipment or expertise that is not available in all areas.
Emerging Diseases
Emerging diseases, such as COVID-19, Ebola, Zika, and SARS, present significant challenges for diagnostics due to their novel and rapidly evolving nature.[7] In order to effectively diagnose and treat emerging diseases, diagnostic tests need to be developed quickly and accurately to detect the specific pathogen causing the disease. One of the challenges in developing diagnostic tests for emerging diseases is the lack of knowledge about the pathogen and its mechanisms of transmission and pathogenesis. This can make it difficult to identify suitable targets for diagnostic tests or develop effective treatments. Another challenge is the need for rapid and accurate diagnostic tests that can be deployed quickly in outbreak settings. Traditional diagnostic testing methods, such as culture-based methods, can take days or weeks to provide results, which can delay diagnosis and treatment. Rapid diagnostic tests that can provide results within hours or minutes are therefore essential for effective management of emerging diseases. What’s more, we have over 10,000 known diseases but diagnostics to only a subset and treatments for fewer still. Newly discovered disease mechanisms and methods to quickly and effectively diagnose rare diseases will continue to drive the need for novel diagnostics.
Emerging Trends in Diagnostics
Point-of-Care Testing
Point-of-care testing (POCT) is a diagnostic testing approach conducted at or near the site of patient care.[8] One of the most promising POCT technologies is the "lab on a chip." These microchips integrate multiple laboratory functions, such as sample preparation, analysis, and detection, onto a small, portable device. This allows for rapid, accurate, and cost-effective testing, especially in resource-limited settings where traditional laboratory equipment is not available. Lab-on-a-chip technology has been applied to various diagnostic tests, including infectious disease testing and cancer detection.
The benefits of POCT include quicker results, cost-effectiveness, and the ability to make treatment decisions in real time. POCT can help to reduce the turnaround time for diagnostic testing, which is particularly important in emergency situations and can also lead to more efficient and effective treatment plans.
The recent COVID-19 pandemic has highlighted the critical importance of accurate and rapid diagnostic testing.[9] With the need to limit the spread of the virus, it was imperative to quickly develop and manufacture tests that could deliver accurate results in a timely manner. In response, the development of antigen tests and nucleic acid amplification tests (NAATs) saw a historic turnaround time, and these tests played a significant role in combating the pandemic. The infrastructure for scaling up the manufacturing of these tests has been validated, and the success in responding to COVID-19 provides valuable lessons for the future. With the lessons learned and the infrastructure in place, we are now better equipped to respond to any future global pandemics.
Wearables
Wearables have transformed the way we monitor and diagnose health conditions. The integration of biosensors and other advanced technologies has enabled wearables to provide accurate and real-time data on various health parameters, including heart rate, blood pressure, and sleeping patterns.[10] This data can be analyzed by healthcare professionals to diagnose and treat a range of health conditions, from chronic diseases to acute illnesses. Wearables also allow patients to take an active role in their healthcare by monitoring their own health and sharing data with healthcare providers. Despite the potential benefits, there are still challenges to be addressed, such as data privacy concerns and the need for more accurate and reliable wearables. Nevertheless, the use of wearables in diagnostics is a promising trend that has the potential to revolutionize the way we approach healthcare.
Wearables are part of a larger concept known as the Internet of Things (IoT), where everyday objects are embedded with sensors and software to create a network for sharing and exchanging data.[11] Examples of household items with IoT technology include fridges, TVs, and laundry machines. In the field of diagnostics, wearables are increasingly being developed with a variety of sensors, such as those in watches, clothing, and jewelry, to provide continuous and real-time monitoring. These wearables have the potential to detect acute conditions such as stroke or heart attacks, providing timely alerts to authorities for faster and more effective treatment.

Genomics
The central dogma of biology postulates that DNA undergoes transcription to RNA, which in turn is translated to proteins. Exploiting this principle to gain a deeper understanding of diseases, humans have developed technologies that allow for meticulous scrutiny of this process. In 2003, the first human genome was completely sequenced,[12] and since then, we have made remarkable strides in developing innovative technologies that offer further insight into various aspects of our genome (DNA), transcriptome (RNA), and proteome (proteins). We have also devised numerous techniques that aid in comprehending intermediate stages, such as genetic and epigenetic modifications, metabolomes, and many more.[13] These pioneering technologies empower healthcare professionals to unravel the mechanisms of disease pathogenesis and identify fresh targets to pursue drug development.
A prominent trend in genomics for diagnostics is the endeavor to quantify genomic profiles at the level of single cells.[14] Given that diverse cells have distinct roles, it is crucial to comprehend the heterogeneous traits that influence downstream molecular dynamics and functionality. Currently, single-cell RNA sequencing (scRNA-seq) is perhaps the most widely used technology that enables researchers to characterize the transcriptome of individual cells.[15] This breakthrough offers the ability to detect specific cellular populations (for instance, within a solid tumor) and quantify their functions, mechanisms, and responses to other cells (such as immune cells).
Genomics is also currently experiencing a trend towards integrating multiple -omic data types to obtain a more comprehensive view of molecular pathways. Although single -omic data can offer valuable insights, multi-omic integration can provide a much more detailed understanding of molecular responses and mechanisms.[16] As -omic technologies continue to advance, data integration with other types of -omic technologies will further enhance our understanding of molecular interactions, pushing us towards the next frontier of genomics research.
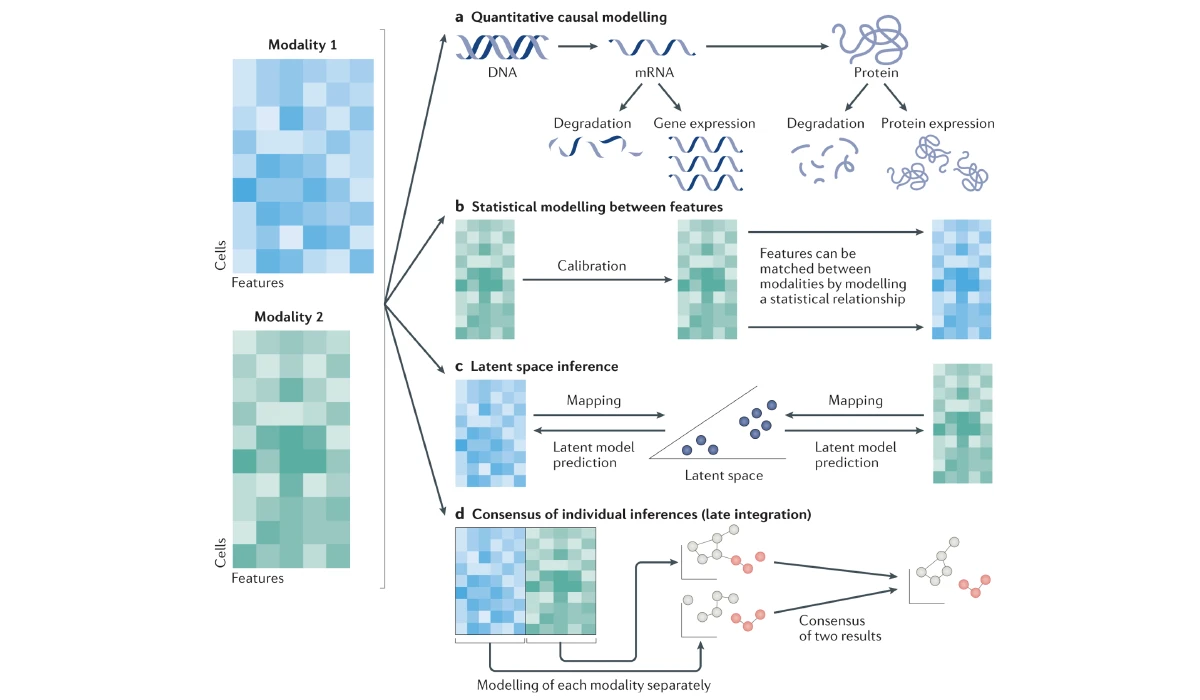
Image source: Multi-Omics Integration in the Age of Million Single-Cell Data, Nature Reviews Nephrology
Artificial Intelligence
Moore's Law is a prediction made by Intel co-founder Gordon Moore in 1965 that the number of transistors on a microchip would double every 18-24 months, leading to an exponential increase in computing power.[17] This prediction has held true for over five decades, and the exponential growth in computing power has had a significant impact on the development of AI, and in particular, the intersection of AI and diagnostics. In radiology, for example, AI algorithms can be used to analyze medical images, such as X-rays and MRIs, and detect abnormalities that may indicate the presence of a disease or condition.[18] AI can also be used to analyze patient data, such as medical history, symptoms, and lab results, and help healthcare providers make more accurate diagnoses.
AI has also been used in clinical decision support (CDS) to help healthcare providers make more informed and accurate decisions about patient care.[19] For example, AI algorithms can analyze patient data, such as medical history, symptoms, and lab results, to suggest potential diagnoses. This can help healthcare providers make more accurate diagnoses and improve patient outcomes. They can also analyze patient data to suggest potential treatments based on the patient's specific characteristics, such as age, gender, and medical history. This can help healthcare providers develop personalized treatment plans that are more effective and have fewer side effects.
As previously mentioned, the field of genomics is undergoing a paradigm shift towards the integration of multiple types of -omic data to provide a more comprehensive understanding of molecular interactions.
AI is emerging as a powerful tool to integrate different modes of data, including text, image, numeric, and multi-omic data, and generate comprehensive results that could potentially lead to more accurate diagnoses and deeper understanding.[20]
For instance, imaging data such as pathology slides can be integrated with gene expression or protein levels to identify molecular changes in tissue structure or function. Similarly, electronic health records can be integrated with imaging or molecular data to elucidate the relationship between cellular or protein level functionality and a phenotype. By facilitating multi-modal data integration, AI offers researchers and clinicians an opportunity to gain a more comprehensive understanding of complex biological systems and develop more effective interventions.
Nanotechnology
Diagnostic nanotechnology involves the use of nanoscale materials and devices for the detection and diagnosis of diseases. Nanotechnology refers to the manipulation and engineering of materials and devices at the nanometer scale, which is approximately 1-100 nanometers.[21] At this scale, the physical and chemical properties of materials can be significantly different from their macro counterparts, making them useful for a range of applications, including medical diagnosis.
Nanotechnology-based diagnostic tools can provide sensitive and accurate detection of disease biomarkers, such as proteins, nucleic acids, and metabolites, that can indicate the presence or progression of a disease. Examples of diagnostic nanotechnology applications include biosensors, nanoparticles, and nanodevices.
Biosensors are devices that detect and measure biological molecules, such as proteins and DNA, by converting their interactions with the analyte into an electrical signal.[22] Biosensors can be made using nanoscale materials, such as carbon nanotubes and nanoparticles, to improve their sensitivity and specificity.
Nanoparticles can be used to deliver drugs or imaging agents to specific tissues or cells in the body. They can also be engineered to specifically target certain biomarkers, such as tumor cells, making them useful for cancer diagnosis and therapy.[23] Nanodevices are miniaturized devices that can be implanted or inserted into the body for real-time monitoring of physiological parameters, such as glucose levels, blood pressure, and heart rate.
Virtual Reality (VR) and Augmented Reality (AR)
Virtual reality (VR) and augmented reality (AR) are technologies that have the potential to revolutionize medical diagnosis and treatment. VR refers to a completely immersive experience that simulates a real-life environment, while AR overlays digital information onto the real-world environment.[24] In the context of medical diagnosis, VR and AR can be used to create realistic simulations of disease processes or anatomical structures to aid in diagnosis and treatment planning. For example, medical students can use VR to practice surgical procedures on a virtual patient, allowing them to gain experience and confidence before operating on a real patient. Surgeons can also use VR to plan complex surgeries and practice them in a virtual environment before performing them on a patient.
AR can be used to overlay information about a patient's anatomy onto their body during surgery, allowing surgeons to see the precise location of structures they need to avoid. AR can also be used to display information about a patient's vital signs or medical history in real time during surgery, helping surgeons make more informed decisions. In addition to diagnosis and treatment, VR and AR can also be used for patient education and rehabilitation. Patients can use VR to learn about their condition and treatment options, as well as to practice rehabilitation exercises in a safe and controlled environment.
Liquid Biopsy
Liquid biopsy is a non-invasive diagnostic technique that involves analyzing a patient's blood, urine, or other bodily fluids for the presence of cancer cells, tumor DNA, or other biomarkers.[25] This approach provides a less invasive and more sensitive method of detecting cancer than traditional tissue biopsies, which can be difficult to perform and may miss important genetic mutations.
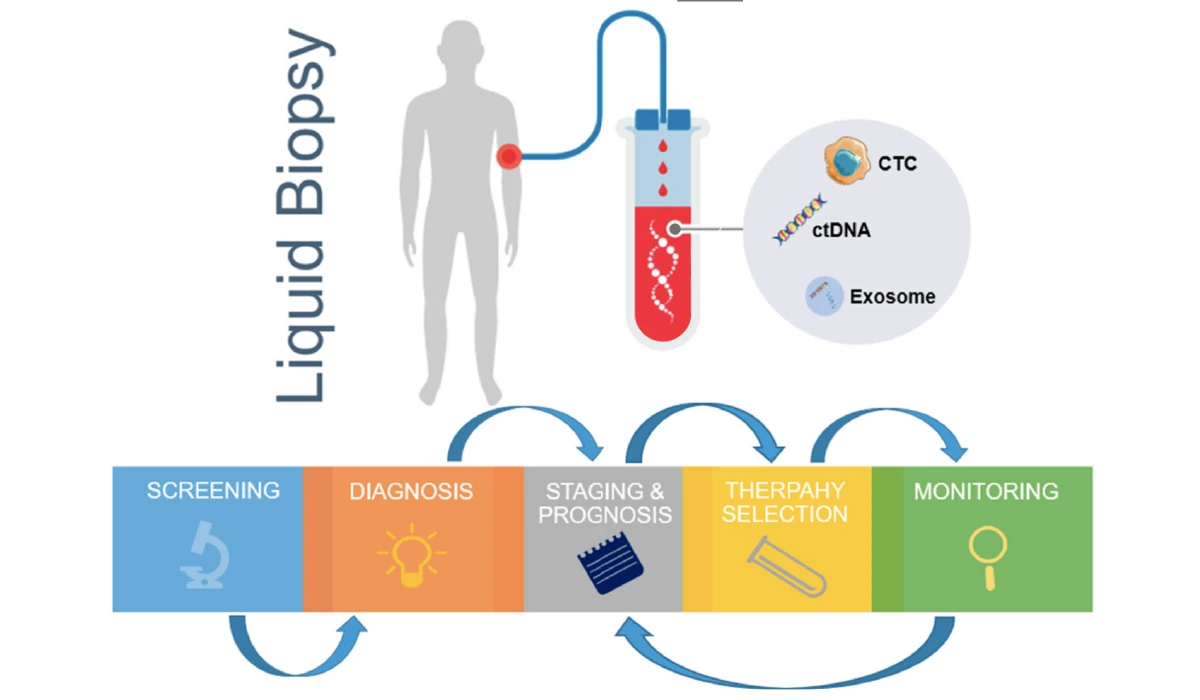
Image source: The Use of Microfluidic Technology for Cancer Applications and Liquid Biopsy, MDPI
Liquid biopsy can be used for early cancer detection, monitoring of disease progression, and identification of treatment-resistant tumors. By analyzing circulating tumor cells (CTCs) or circulating tumor DNA (ctDNA) in a patient's blood, liquid biopsy can provide real-time information on the genetic changes occurring in a tumor, allowing for personalized treatment strategies.
Liquid biopsy is also being explored for other applications beyond cancer diagnosis. For example, it can be used to monitor infectious diseases, such as HIV and hepatitis, by detecting viral DNA or RNA in the blood. Liquid biopsy can also be used for prenatal testing by analyzing fetal DNA in maternal blood.
Democratization and Decentralization
Democratization refers to the process of making something, such as a service, technology, or knowledge, accessible and available to a wider and more diverse group of people. It is often associated with promoting equality and breaking down barriers that prevent certain groups from accessing resources or opportunities. Decentralization refers to the transfer of power, authority, or decision-making from a central authority or organization to a distributed network of individuals, groups, or local entities.
In the context of diagnostics, democratization and decentralization refer to making diagnostic tools and technologies more widely accessible to patients and healthcare providers, regardless of their geographic location, socioeconomic status, or level of technical expertise.[26]
This can involve the development of point-of-care diagnostic tools that are affordable, easy to use, and do not require specialized laboratory equipment or trained personnel. It can also involve the use of telemedicine and other digital health technologies to bring diagnostic services to remote or underserved communities.

Democratization and decentralization of diagnostics can have several benefits, including improving access to timely and accurate diagnoses, reducing healthcare costs, and increasing patient engagement in their own healthcare. For instance, point-of-care diagnostic tests can provide immediate results, allowing for faster diagnosis and treatment decisions, which can be particularly important in emergency situations or in resource-limited settings. Telemedicine can enable patients to receive diagnostic services from the comfort of their own homes, reducing the need for in-person visits and lowering healthcare costs. Overall, democratization of diagnostics can improve healthcare outcomes and promote equity in access to healthcare services.
Automation
Automation is playing an increasingly important role in the field of diagnostics. Automating diagnostic workflows can increase efficiency, reduce errors, and improve safety issues.[27] Automation can be used to handle and process samples in a diagnostic laboratory. This can include automated sample preparation, automated pipetting, and automated sample labeling. It can also be used for testing and analysis in a diagnostic laboratory. This can include automated microscopy, automated immunoassays, and automated PCR machines. Lastly, quality control can also be automated by using sensors for error detection as well as maintenance and calibration of equipment.
Market Outlook
The COVID-19 pandemic has shed light on the crucial importance of rapid and accurate diagnostic tools. According to a recent report by Precedence Research, the global diagnostics market was valued at $179 billion in 2022, with North America leading in revenue share.[28] The report also forecasts that the market will expand to $348 billion by 2030, largely driven by the prevalence of chronic diseases. However, while it is true that chronic illness will contribute to the growth of the diagnostics market, there are several looming issues that are likely to fuel its further expansion.
Aging-Related Diseases
The world's population is undergoing a significant demographic shift, with medical advancements and low birth rates contributing to an older median age. This trend is likely to lead to an increase in aging-related ailments, including hearing loss, cataracts, refractive errors, back and neck pain, osteoarthritis, chronic obstructive pulmonary disease, diabetes, depression, and dementia.[29] With new findings emerging about the correlation between aging and inflammation, more advanced molecular diagnostic tools will likely be developed to identify phenotypes triggered by these inflammatory pathways.
Mental Health Epidemic
The COVID-19 pandemic has brought into sharp focus the alarming rise of the global mental health crisis and the loneliness epidemic. Social isolation, loss of loved ones, economic uncertainty, and the disruption of daily routines have significantly impacted people's mental well-being, aggravating pre-existing mental health conditions. As a result, anxiety, depression, and suicidal ideation have surged worldwide.[30] However, the current diagnosis of mental health issues is symptom-based, which could lead to subjective interpretation and misdiagnosis.
Future efforts must prioritize identifying clear clinical or biological markers for diagnosis to standardize patient care in mental health and mitigate the long-term impact of this crisis.
Climate-Related Diseases
As a result of the ongoing climate change, vectors such as mosquitoes and ticks that transmit diseases may have more extended periods to reproduce and spread infections.[31] Additionally, changing weather patterns have led to forced migration of animals, which could lead to novel contact patterns between animals and humans, resulting in new disease outbreaks. The expansion of fungi into warmer regions previously unsuitable for their growth, coupled with the unknown effects of rising temperatures and water levels, could also create new disease indications that will require real-time diagnosis to prevent future pandemics.
Antimicrobial Resistance
Antimicrobial resistance remains a persistent concern in clinical settings, as patients with undiagnosed infections may receive inappropriate treatments, hindering their recovery and promoting further selective pressure for pathogen mutations.[32] The development of novel diagnostic tools capable of providing rapid, point-of-care identification of infectious agents is crucial in guiding effective treatment strategies. By accurately identifying the specific pathogen responsible for an infection, clinicians can choose the appropriate antibiotic or antiviral agent to treat it, thereby improving patient outcomes and reducing the selective pressure for antibiotic-resistant strains to emerge.
Conclusion
In conclusion, diagnostics are a crucial component of modern healthcare, enabling early detection, accurate diagnosis, and effective treatment of a wide range of medical conditions. Advances in technology, such as liquid biopsies, AI and machine learning, and non-invasive diagnostic techniques, are rapidly transforming the field of diagnostics, making it more accessible, accurate, and efficient than ever before. With the growing demand for personalized and precision medicine, the role of diagnostics in healthcare will continue to grow in importance, helping clinicians to deliver more targeted and effective treatments to patients. As we look to the future, diagnostics will play an increasingly important role in improving patient outcomes and advancing medical research, paving the way for a healthier and more prosperous society.
Landscape
Point-of-Care Testing
SIME
Aplife Biotech
OraLiva
Spectra Plasmonics
Novascan
Wearables
Mindera Health
Strados Labs
Inner Cosmos
Atmo Biosciences
Genomics
Pepper Bio
Artificial Intelligence
Hume.ai
Antiverse
Nanotechnology
Starpax Biopharma
Neobe Therapeutics
Democratization and Decentralization
Sampling Human
Zafrens
Novel Microdevices
Automation
Nanopec
Celtro
References
[1] Berger D, A Brief History of Medical Diagnosis and the Birth of the Clinical Laboratory, Part 1--Ancient times through the 19th century, MLO Med Lab Obs, 1999 Jul;31(7):28-30, 32, 34-40, PMID: 10539661
[2] Lens Crafters Circa 1590: Invention of the Microscope, APS News
[3] How Did We Get the Stethoscope?, American Lung Association
[4] Promoting Cancer Early Diagnosis, World Health Organization
[5] Šimundić AM, Measures of Diagnostic Accuracy: Basic Definitions, EJIFCC, 2009 Jan 20;19(4):203-11, PMID: 27683318; PMCID: PMC4975285
[6] A Grim Diagnosis - Half The World’s Population Has Limited Access To Diagnostics, Forbes
[7] Ogden NH, AbdelMalik P, Pulliam J. Emerging Infectious Diseases: Prediction and Detection, Can Commun Dis Rep, 2017 Oct 5;43(10):206-211, doi: 10.14745/ccdr.v43i10a03, PMID: 29770047; PMCID: PMC5764723
[8] Vashist SK, Point-of-Care Diagnostics: Recent Advances and Trends, Biosensors (Basel), 2017 Dec 18;7(4):62, doi: 10.3390/bios7040062, PMID: 29258285; PMCID: PMC5746785
[9] Drain PK, Rapid Diagnostic Testing for SARS-CoV-2, N Engl J Med, 2022 Jan 20;386(3):264-272, doi: 10.1056/NEJMcp2117115, Epub 2022 Jan 7, PMID: 34995029; PMCID: PMC8820190
[10] Chakrabarti S, Biswas N, Jones LD, Kesari S, Ashili S, Smart Consumer Wearables as Digital Diagnostic Tools: A Review, Diagnostics, 2022; 12(9):2110, https://doi.org/10.3390/diagnostics12092110
[11] Haghi M, Thurow K, Stoll R, Wearable Devices in Medical Internet of Things: Scientific Research and Commercially Available Devices, Healthc Inform Res, 2017 Jan;23(1):4-15, doi: 10.4258/hir.2017.23.1.4, Epub 2017 Jan 31, PMID: 28261526; PMCID: PMC5334130
[12] Lander ES, Linton LM, Birren B, Nusbaum C, Zody MC, Baldwin J, Devon K, Dewar K, Collins F, Guyer MS, Peterson J, Felsenfeld A, Wetterstrand KA, Patrinos A, Morgan MJ, de Jong P, Catanese JJ, Osoegawa K, Shizuya H, Choi S, Chen YJ, Szustakowki J; International Human Genome Sequencing Consortium, Initial Sequencing and Analysis of The Human Genome, Nature, 2001 Feb 15;409(6822):860-921, doi: 10.1038/35057062, Erratum in: Nature 2001 Aug 2;412(6846):565, Erratum in: Nature 2001 Jun 7;411(6838):720, Szustakowki, J [corrected to Szustakowski, J], PMID: 11237011
[13] Collins FS, Doudna JA, Lander ES, Rotimi CN, Human Molecular Genetics and Genomics - Impo,tant Advances and Exciting Possibilities, N Engl J Med, 2021 Jan 7;384(1):1-4, doi: 10.1056/NEJMp2030694. Epub 2021 Jan 2. PMID: 33393745
[14] de Wreede LC, Schetelig J, Putter H, Analysis of Survival Outcomes in Haematopoietic Cell Transplant Studies: Pitfalls and Solutions, Bone Marrow Transplant, 2022 Sep;57(9):1428-1434, doi: 10.1038/s41409-022-01740-4, Epub 2022 Jun 27, PMID: 35760893
[15] Hwang B, Lee JH, Bang D, Single-cell RNA Sequencing Technologies and Bioinformatics Pipelines, Exp Mol Med, 2018 Aug 7;50(8):1-14, doi: 10.1038/s12276-018-0071-8, Erratum in: Exp Mol Med, 2021 May;53(5):1005, PMID: 30089861; PMCID: PMC6082860
[16] Miao Z, Humphreys BD, McMahon AP, Kim J, Multi-Omics Integration in The Age of Million Single-Cell Data, Nat Rev Nephrol, 2021 Nov;17(11):710-724, doi: 10.1038/s41581-021-00463-x, Epub 2021 Aug 20, PMID: 34417589; PMCID: PMC9191639
[17] What is Moore’s Law?, Our World in Data
[18] How AI Is Changing Medical Imaging to Improve Patient Care, TIME
[19] Giordano C, Brennan M, Mohamed B, Rashidi P, Modave F, Tighe P, Accessing Artificial Intelligence for Clinical Decision-Making, Front Digit Health, 2021 Jun 25;3:645232, doi: 10.3389/fdgth.2021.645232, PMID: 34713115; PMCID: PMC8521931
[20] Lipkova J, Chen RJ, Chen B, Lu MY, Barbieri M, Shao D, Vaidya AJ, Chen C, Zhuang L, Williamson DFK, Shaban M, Chen TY, Mahmood F, Artificial Intelligence for Multimodal Data Integration in Oncologym Cancer Cell, 2022 Oct 10;40(10):1095-1110, doi: 10.1016/j.ccell.2022.09.012, PMID: 36220072
[21] Earlier Detection and Diagnosis, National Cancer Institute
[22] Bhalla N, Pan Y, Yang Z, Payam AF, Opportunities and Challenges for Biosensors and Nanoscale Analytical Tools for Pandemics: COVID-19. ACS Nano, 2020 Jul 28;14(7):7783-7807, doi: 10.1021/acsnano.0c04421, Epub 2020 Jun 26, PMID: 32551559; PMCID: PMC7319134
[23] Baetke SC, Lammers T, Kiessling F, Applications of Nanoparticles for Diagnosis and Therapy of Cancer, Br J Radiol, 2015 Oct;88(1054):20150207, doi: 10.1259/bjr.20150207, Epub 2015 Jun 12, PMID: 25969868; PMCID: PMC4630860
[24] Augmented Reality and Virtual Reality in Medical Devices, Digital Health Center of Excellence, FDA
[25] Liquid Biopsy, Cleaveland Clinic
[26] Abou Tayoun AN, Burchard PR, Malik I, Scherer A, Tsongalis GJ, Democratizing Molecular Diagnostics for the Developing World, Am J Clin Pathol, 2014 Jan;141(1):17-24, doi: 10.1309/AJCPA1L4KPXBJNPG, PMID: 24343733
[27] Holland I, Davies JA, Automation in the Life Science Research Laboratory, Front Bioeng Biotechnol, 2020 Nov 13;8:571777, doi: 10.3389/fbioe.2020.571777, PMID: 33282848; PMCID: PMC7691657
[28] Diagnostic Testing Market Size to Hit USD 348.75 Bn by 2030, Precedence Research, Globe Newswire
[29] Aging and health, World Health Organization
[30] Mental Health During the COVID-19 Pandemic, National Institutes of Health
[31] Climate Change and Infectious Diseases, Centers for Disease Control and Prevention
[32] Vasala A, Hytönen VP, Laitinen OH, Modern Tools for Rapid Diagnostics of Antimicrobial Resistance, Front Cell Infect Microbiol, 2020 Jul 15;10:308, doi: 10.3389/fcimb.2020.00308, PMID: 32760676; PMCID: PMC7373752
